Piece of Cake: DKA/HHS Update Part II
Contributor: Dillon Warr, MD and Jason Hine, MD
Guest: George Willis, MD, FACEP
Welcome to our Part II of our talk with Dr. George Willis, the endocrine expert, on Diabetic Ketoacidosis (DKA) and Hyperosmolar Hyperglycemia State (HHS). In it we review The American Diabetes Association consensus report. In Part I, we discussed epidemiology, pathophysiology, and clinical presentation of DKA/HHS. Check out Part 1 HERE.
In Part II, we continue our deep dive into with a focus on diagnostic criteria updates and new
treatment guidelines. We break down the latest consensus statement and
discuss how these changes impact clinical practice.
Keeping your skills up in rare procedures is an uphill battle. Let SimKit do all the heavy lifting with simulation training that delivers to your door once a month. Use coupon code SimKit10 for 10% off
Key Points
- The diagnostic criteria for DKA have changed, with lower glucose cutoffs and beta-hydroxybutyrate as the preferred ketone marker.
- Fluids matter! Balanced solutions like LR and Plasma-Lyte are now first-line choices.
- Subcutaneous insulin protocols (SQUID protocol) are the new hotness in DKA management and can reduce ICU admissions.
- Early basal insulin can improve transitions off IV insulin.
- Electrolyte management, especially potassium, remains critical in avoiding complications.
Diagnosis
Diagnostic Criteria Updates
- The glucose threshold for DKA diagnosis lowered from 250 mg/dL to 200 mg/dL
- Recognition of euglycemic DKA in patients with low glucose levels but meeting other criteria
- Beta-hydroxybutyrate included in the diagnostic workup as the preferred ketone body marker
- For the acidosis, the criteria are pH < 7.3 or bicarb < 18
- Serum osmolarity calculations now a recognized tool for diagnosing Hyperosmolar Hyperglycemic State (HHS)
- The concensus statement has a great graphic reproduced below that should be added to your peripheral brain (smart phone) for quick reference:
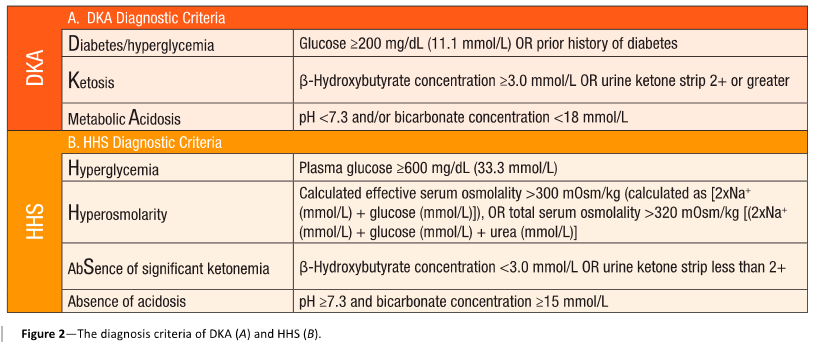
Lab Testing & Initial Workup
- Standard lab panel includes glucose, electrolytes, anion gap, beta-hydroxybutyrate, and VBG.
- End-tidal CO2 > 27 mmHg may help rule out DKA quickly
- Importance of differentiating DKA from HHS based on sodium, pH, bicarbonate, and ketones
Treatment
Fluid Resuscitation
- Balanced crystalloids (LR, Plasma-Lyte) now recommended over normal saline
- Adjustments for patients at risk of fluid overload (CHF, renal failure)
Insulin Therapy
- Bolus insulin no longer recommended before starting an insulin infusion. This practice has been common but is now census supported.
- For HHS, 0.05 u/kg/hr is a great start. For DKA, it is 0.1 u/kg/hr as a standard start.
- New option for subcutaneous insulin in mild-moderate DKA using the SQUID protocol
- Early initiation of basal insulin to improve transition off IV insulin
Potassium Management
New potassium replacement guidelines:
- >5.0 mEq/L: Start insulin without supplementation
- 3.5–5.0 mEq/L: Start insulin + potassium replacement
- <3.5 mEq/L: Delay insulin, aggressively replace potassium
Other Electrolytes and Considerations
- Phosphorus supplementation only if symptomatic
- Allowing patients to eat during treatment if tolerated
- The major risks to these patients in treatment are hypoglycemia and hypokalemia. Beware this issues and allow the patient to eat for repletions.
- For pediatric patients, beware cerebral edema
- HHS is a slow process to happen and should be a slow one to fix. They all should be admitted to the ICU.
References
Umpierrez GE, Davis GM, ElSayed NA, et al. Hyperglycaemic crises in adults with diabetes: a consensus report. Diabetologia. 2024;67(8):1455-1479. [pubmed]
Griffey RT, Schneider RM, Girardi M, Yeary J, McCammon C, Frawley L, Ancona R, Cruz-Bravo P. The SQuID protocol (subcutaneous insulin in diabetic ketoacidosis): Impacts on ED operational metrics. Acad Emerg Med. 2023 Aug;30(8):800-808. doi: 10.1111/acem.14685. Epub 2023 Feb 27. PMID: 36775281. [pubmed]
Hunter C, Putman M, Foster J, Souers A, Rodriguez A, Zuver C, Papa L. Utilizing End-Tidal Carbon Dioxide to Diagnose Diabetic Ketoacidosis in Prehospital Patients with Hyperglycemia. Prehosp Disaster Med. 2020 Jun;35(3):281-284. [pubmed]


